Women And Children In India Are Suffering From High Rates Of Anemia
Women and children in India suffer from anemia more than most other countries in the world. A staggering 58% of children, 53% of non-pregnant women, and 50% of pregnant women are anemic. However, other estimates suggest these numbers could be even higher (as we’ll explore later in this post). Anemia is a serious issue that can be debilitating for those affected. It’s high time we shine a light on this problem if we want to safeguard the well-being of future generations.
In this post, we’ll first delve into the numbers to demonstrate that India is indeed silently grappling with this massive issue. Next, we’ll examine the causes of anemia in India and how it severely impacts women and children. Finally, we’ll discuss India’s attempts to address the problem with limited success and propose more effective approaches to tackle it.
So, let’s dive right in!
Anemia in India: Let’s look at the numbers
The numbers paint a grim picture when it comes to anemia in Indian women and children. According to the National Family Health Survey (NFHS-4), 58% of children aged 6-59 months, 53% of non-pregnant women aged 15-49 years, and 50% of pregnant women are anemic. If we consider children between ages 12-23 months, then 80% are anemic. These figures are alarming, but they don’t even tell the whole story.
A more recent study reveals that the situation is even worse if we include non-iron deficient anemia (NIDA), where a person is anemic without being iron deficient. Two-thirds of all reproductive-aged women suffer from anemia if we include NIDA.
Furthermore, it’s not just limited to rural areas where poverty is rampant; urban areas which are generally more affluent also have record high rates of anemia.
India’s anemia rates are much higher than those in many other countries, such as the United States, China, and even some neighboring or African countries. For example, 53% of women of reproductive age are anemic in India compared to 10% in the United States, 30% in China, 42% in Bangladesh, and 38% in Ghana.
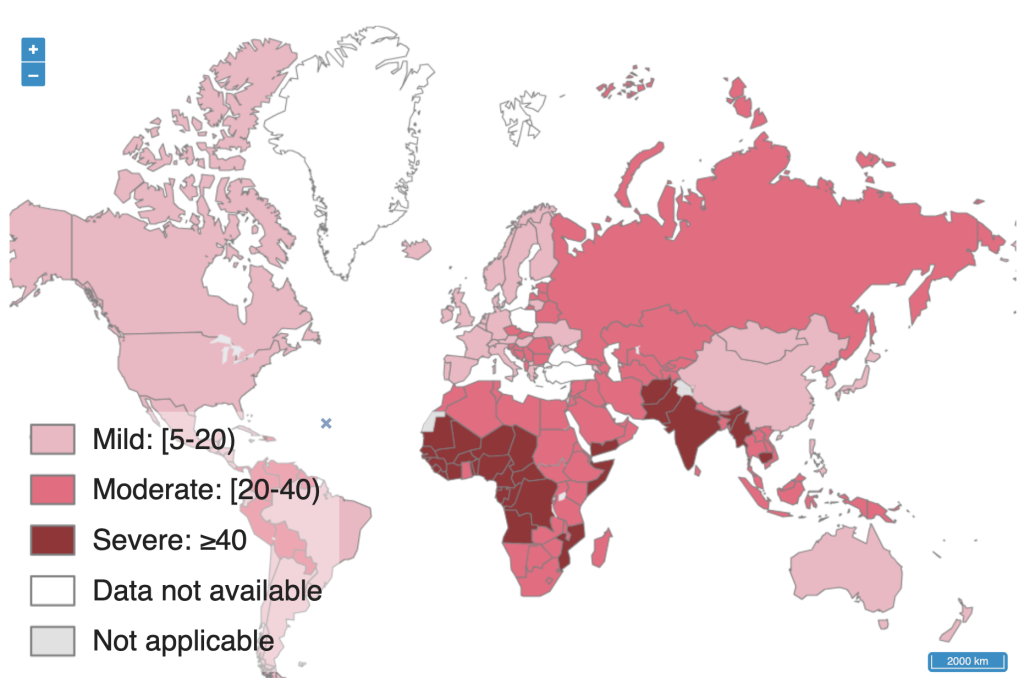
Aside from countries in Sub-Saharan Africa, India is at the top of the list for children with anemia.
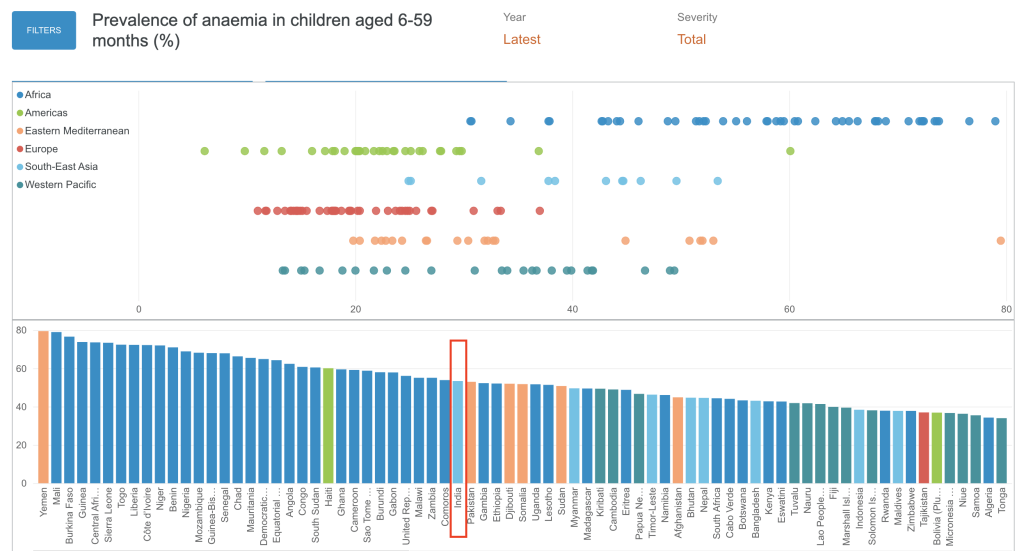
Either way, the numbers are scary high. In the next section, we’ll delve deeper into how the anemia crisis is impacting Indian women and young children and explore the root causes behind this widespread problem.
How Does Anemia Impact People in India?
Poor Pregnancy Outcomes
Lactating and pregnant women in India have the highest levels of anemia. Anemia during pregnancy is dangerous because it can lead to low birthweight (which can cause stunted growth, cognitive development issues, and increased risk of infections) and preterm labor. An undernourished mother gives birth to an undernourished baby, perpetuating an intergenerational cycle of undernutrition.
Anemia in expectant mothers also increases the risk of perinatal mortality – the death of a fetus or newborn within one week after birth. This is due to inadequate oxygen supply from low hemoglobin levels in the blood.
Maternal Mortality
India’s maternal mortality rate (MMR) is one of the highest in the world. Many of these maternal deaths are caused by anemia.
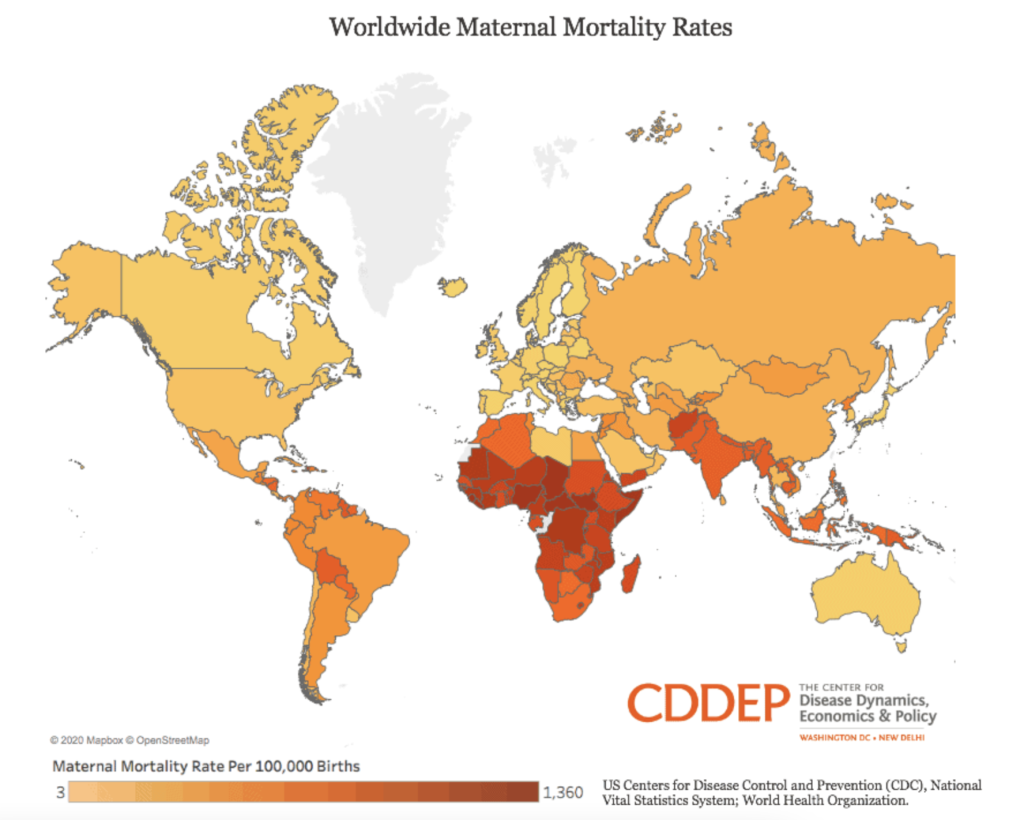
Stunted children
34% of children in India have stunted growth. A major cause of this is malnutrition and anemia. It’s known that 50% of growth failure occurring by the age of two actually begins in the womb due to poor nutrition before and during pregnancy. As a result, anemic mothers give birth to anemic children, who then have stunted growth.
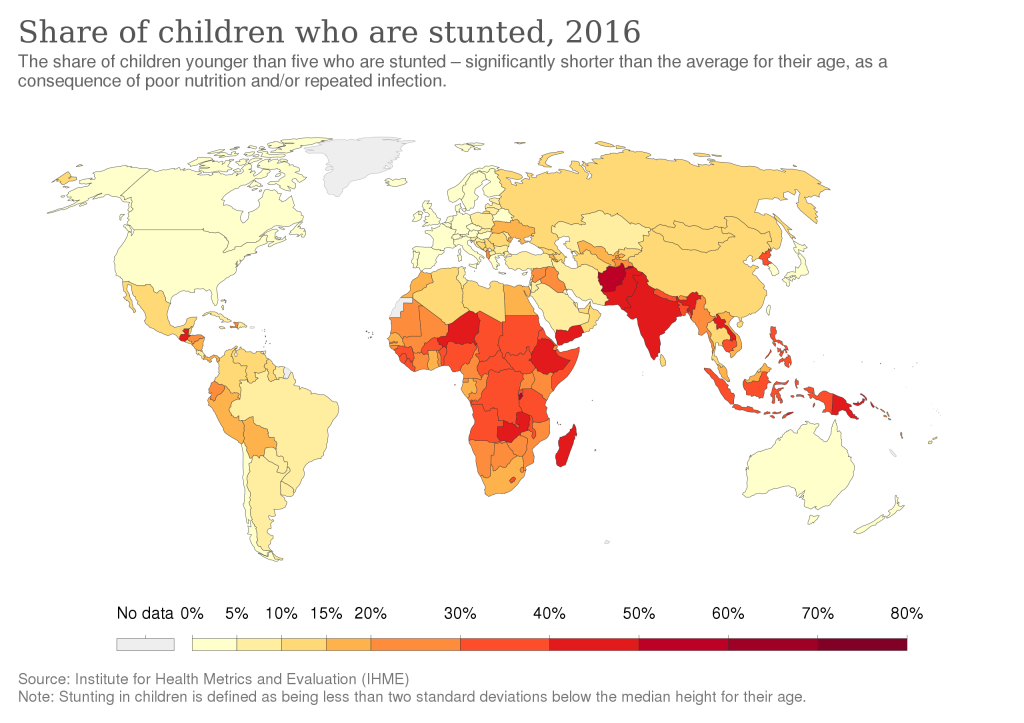
Disability
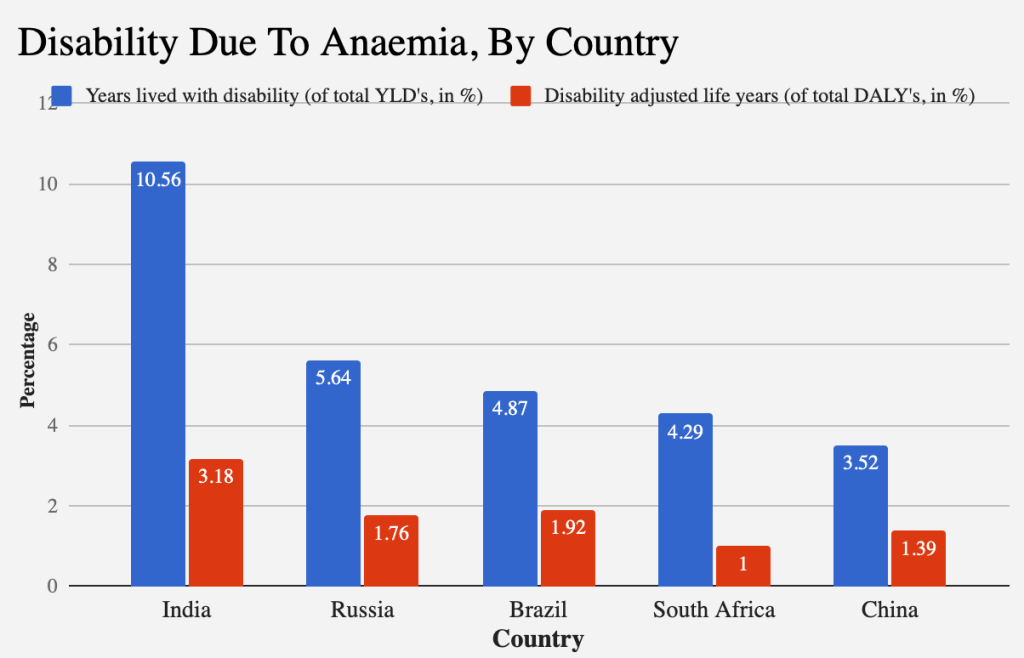
According to a 2002 study published in the Journal of Nutrition, anemia led to a 17% loss in productivity among workers engaged in heavy physical labor and a 5% dip in the output of moderately active workers. India loses 0.9% of its gross domestic product (GDP) due to iron-deficiency anemia, as reported in a 2003 paper published in Food Policy. This translates to a loss of up to $20.25 billion (Rs.1.35 lakh crore).
What’s more, iron-deficiency anemia has been the leading cause of disability in India for over a decade. Iron deficiency accounts for over 10% of all “Years Lived with Disability” among Indians. In this context, disability refers to the absence of good health, encompassing loss of mobility, self-care, participation in routine activities, pain and discomfort, anxiety and depression, and cognitive impairment.
Reduced IQ and cognitive development
Children born to anemic mothers have delayed cognitive development because they aren’t getting enough oxygen to support proper brain growth and development. It also impacts language skills, motor skills and coordination, and can even reduces IQ by up to 10 points. And worst of all, the effects of iron deficiency in infancy cannot be corrected by subsequent iron therapy.
Mental illness
Iron deficiency can increase the risk of psychiatric disorders (eg. autism, anxiety, depression, bipolar disorder, etc) and lead to impaired neurocognitive functions (eg. poor memory and slower neural processing). This is because the central nervous system is highly dependent on iron-containing enzymes and proteins. Deficiency of iron in early childhood further increases the risk of psychiatric issues.
Poor cardiac health
Severe iron deficiency can lead to cardiac and skeletal myopathy, which is why it’s common in patients with cardiovascular disease. In fact, up to 60% of patients with coronary artery disease, and an even higher proportion of those with heart failure or pulmonary hypertension, have iron deficiency.
This is because iron deficiency increases oxidative stress and weakens the cardiac muscle, making a person more prone to cardiac issues.
In summary, there are countless papers and studies that highlight the detrimental effects of anemia and iron deficiency. The points I’ve mentioned above barely scratch the surface. Anemia is a serious issue that leads to poor health, and it’s honestly quite scary that so many women and children in India are affected by it.
What Is Causing Such Widespread Anemia In India?
Diet
The main cause of anemia is not getting enough iron and other essential nutrients from food. Considering that 40% of Indians are vegetarians and 80% of the population avoids meat most of the time, it’s no wonder they’re more prone to anemia. Getting enough iron on a vegetarian diet can be quite tricky.
To understand why, we need to know that not all iron is created equal. There are two types: Heme and Non-heme. Animal foods contain heme iron, while plant foods have non-heme iron.
Non-heme iron is less bioavailable because it contains compounds (like phytate, oxalate, and polyphenols) that inhibit iron absorption. For example, whole grains, legumes, and nuts have phytate, which is a powerful iron absorption blocker. Yet, for vegetarians, grain products are their main source of dietary iron.
What’s more, since most of India bans beef consumption, Indians miss out on one of the best sources of iron. Kerala, however, is an exception. It has the lowest rates of anemia in the country and is one of the few Indian states where beef is legal. Meanwhile, some of the highest prevalence of anaemia is in the north, northeast, and central states, which have a much larger vegetarian population. Coincidence? Possible. But interesting none the less.
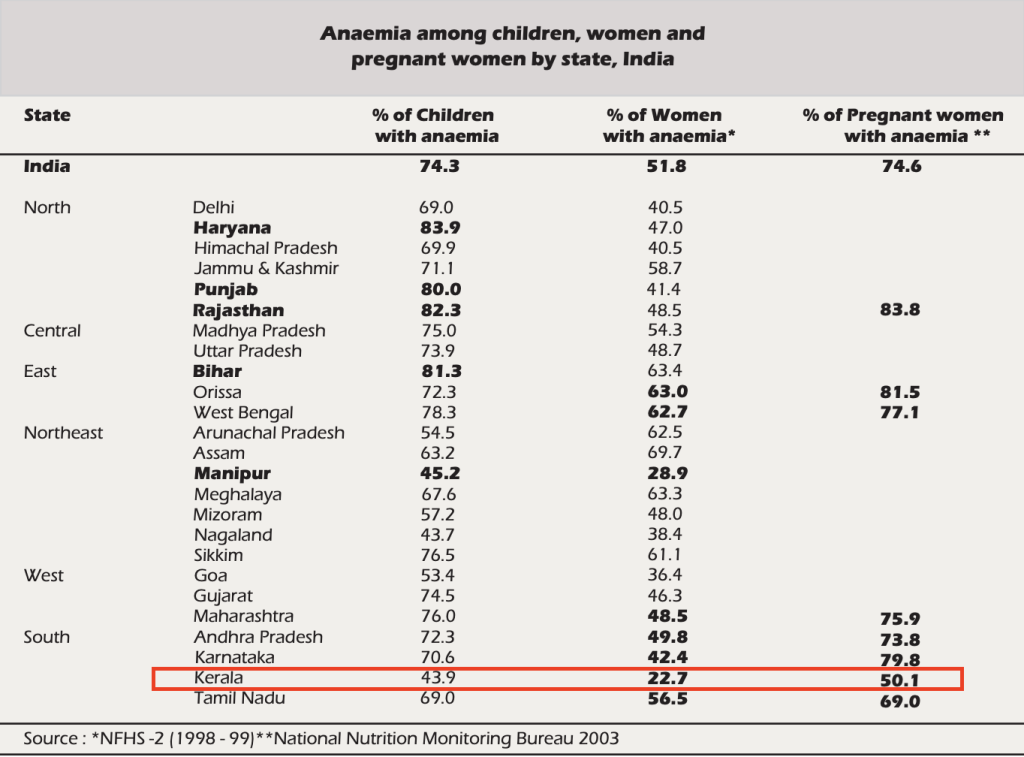
Also, having too much coffee, tea, or calcium in your diet can affect iron absorption. Many Indians rely on dairy as their primary protein source while following a vegetarian diet. Combining high calcium intake with vegetarian foods that contain iron inhibitors might be another reason for poor iron stores.
Poverty
The high rates of poverty in India naturally lead to less calories and nutrition in people’s diets. In fact, more than 20% of Indian women are malnourished. Micronutrient deficiencies, such as folate, B12, and vitamin A, can contribute to anemia. So, if a woman or child isn’t getting enough calories to begin with, there’s a high chance they’re not getting enough iron either.
Pollution
Anyone who’s visited India knows that air pollution is a huge issue in every urban city. But did you know that long-term exposure to air pollution can lead to anemia? This happens because it triggers systemic inflammation. One study revealed that for every 10 µg/m3 increase in ambient PM 2.5 exposure (a type of air pollution), the average anemia prevalence among Indians rises by 7.23%.
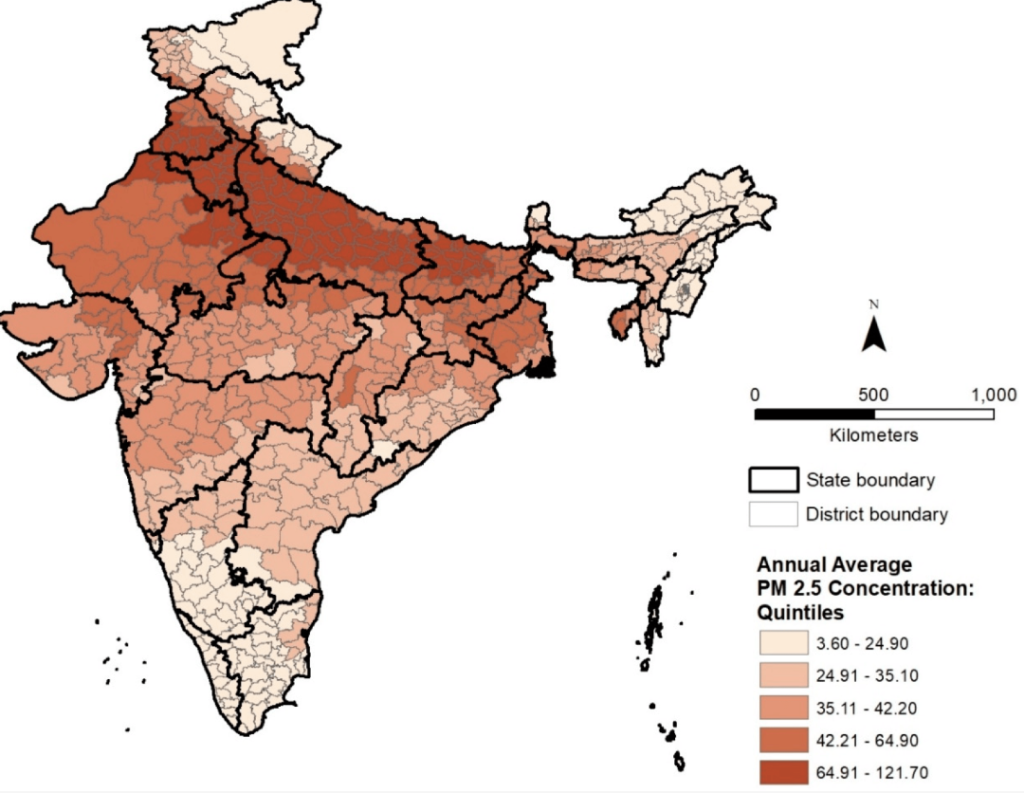
It’s not often that people link pollution to anemia, but it could very well explain why so many Indians are affected. Environment does play a big role in our health, after all.
Infections
Various parasitic infections and infectious diseases, such as H. Pylori, HIV, Malaria, and worm infestation, can contribute to anemia. This happens because infections affect the gut microbiome, which then influences the amount of iron our bodies can absorb.
In India, infections are more prevalent due to poor hygiene standards and unsafe drinking water in many regions of the country.
Other theories
A few other causes of anemia include chronic inflammation (e.g., celiac disease), chronic blood loss (e.g., excessive periods), surgery, injuries, accidents, and the use of intrauterine devices, anticoagulants, or antiplatelets. However, these likely aren’t the primary causes of anemia in Indians. The more probable explanations are diet, malnourishment, pollution, and infections.
How Is India Solving The Anemia Crisis?
The Indian government is well aware of the high prevalence of anemia and has launched several initiatives to reduce it. For instance:
National Iron+ Initiative
In 2013, the government of India launched the National Iron+ Initiative, where they distributed free iron folic acid tablets to iron-deficient women, adolescent girls, and young children.
However, the intervention was poorly managed and lacked supervision. Health providers received little to no training on the initiative’s purpose and strategy, and the program wasn’t even halfway implemented. As a result, some women got the tablets, while others missed out.
Anemia Mukt Bharat
The Anemia Mukt Bharat (Anemia-Free India) strategy, introduced in 2018, aimed to tackle anemia with six interventions: IFA supplementation, deworming, food fortification, improved access to healthcare services, and treatment of anemia cases.
Despite being a more focused effort, it didn’t make a significant dent in anemia rates.
POSHAN Abhiyaan
Launched in 2018 by the Ministry of Women and Child Development, POSHAN Abhiyaan aimed to tackle malnutrition in India by focusing on nutrition for children under six years old and pregnant and lactating mothers. Their approach was to fortify certain foods and promote healthy dietary practices.
Despite these efforts over the past decade, there has been limited progress; national anemia rates have experienced only a marginal decline.
Firstly, these initiatives are prescriptive rather than preventative. Interventions should occur in the first 1,000 days of life (270 days of pregnancy and 730 days 0-24 months), which is the “window of opportunity.” We haven’t focused on preventing undernutrition when it matters most – in the womb. Instead, we are addressing women and children after much of the damage has already occurred.
Secondly, the initiatives targeted iron deficiency anemia but didn’t diagnose or treat women with non-iron deficient anemia. Non-iron deficient anemia cannot be treated by simply providing more iron. A more holistic approach to nutrition is needed.
Lastly, offering weekly iron supplements and fortifying food is not enough. For one, relying on iron tablets as a long-term strategy can be harmful – iron supplements are known to impact the gut microbiome and may lead to issues like colon cancer if taken for extended periods. Secondly, iron tablets don’t address the root cause of anemia. Anemia is a multi-factorial problem, where not only iron but also other factors and nutritional deficiencies play significant roles.
So what is the way forward?
How Do We Reduce Anemia In India?
To tackle the prevalence of anemia in India, we must address the root causes. We should focus on proper diet (especially before and during pregnancy), tackling pollution, improving sanitation, and reducing malnutrition.
The country needs:
1) Improved Public Health Infrastructure
Access to quality healthcare services has to exist, particularly in rural areas, so we can diagnose and treat anemia early. Many people in India suffer from moderate anaemia in silence, only for it to turn into severe anaemia and become much harder to treat.
2) Nutritional Education and Awareness
We need to educate women and young mothers about the importance of a balanced diet, iron-rich foods, and proper food preparation techniques to boost iron absorption. Additionally, promoting the benefits of animal-based foods (for non-vegetarian Indians) is essential.
A top-down approach alone isn’t enough either. We can also adopt a bottom-up approach by educating and promoting an iron-rich diet among our Indian friends and family.
3) Addressing Environmental and Sanitation Issues
Pollution levels across the country have to go down. The Indian government is implementing regulations and has set up sustainable development goals, but it’s unclear if there’s a sense of urgency to resolve the issue. Furthermore, the government should invest in proper sanitation infrastructure to ensure people have access to safe drinking water.
Conclusion
I hope you found this post informative. I certainly learned a lot while researching it, and I hope you did too. As always, if you have any questions or comments, feel free to reply and share in the comments below.







Your posts on the state of Indian health and nutrition are too good. Subscribed to receive more in-depth, well-researched takes 🙂
thank you!